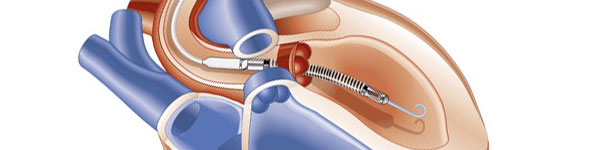
Placement of a pulmonary artery catheter (PAC), commonly known as a Swan-Ganz catheter, provides hemodynamic data that is vital for clinicians treating patients with acute decompensated heart failure or cardiogenic shock. While routine use has been shown to not be beneficial, there are many instances in which hemodynamic monitoring through the use of a Swan is highly indicated.
“Hemodynamic monitoring by PAC or the Swan-Ganz is a diagnostic tool that by itself cannot improve a patient’s condition,” says Cesar Y. Guerrero-Miranda, MD, FACC, Medical Director, Mechanical Circulatory Support, Advanced Heart Failure and Transplant Cardiology, Baylor University Medical Center, part of Baylor Scott & White Health. “The focus must not be whether PAC use is associated with better outcomes, but how to translate the hemodynamic information obtained from PAC into appropriate interventions and therapies that lead to better outcomes.”
Who needs a Swan?
The 2013 American College of Cardiology/American Heart Association heart failure guidelines outline the clinical conditions in which a Swan-Ganz catheter is indicated or should be considered, and when it is not recommended:
- Routine use of invasive hemodynamic monitoring is not recommended in normotensive patients with acute decompensated heart failure and congestion who are responsive to diuretics and vasodilators. In these cases, a Swan-Ganz catheter is not needed to guide therapy.
- Invasive hemodynamic monitoring is recommended in patients with respiratory distress or in patients with clinical evidence of impaired perfusion in whom the adequacy or excess of intra-cardiac filling pressures cannot be determined from clinical assessment and measurement of cardiac output to determinate circulatory perfusion is necessary.
- Invasive hemodynamic monitoring should be considered in a patient:
- Who is refractory to initial therapy,
- Whose volume status and cardiac filling pressures are unclear or difficult to find,
- Who has clinically significant hypotension (typically SBP < 80 mm Hg) or worsening renal function during therapy,
- Who has probable pulmonary hypertension, assessed by echocardiography, to confirm the diagnosis and assess its reversibility,
- Who has been considering the diagnosis of restrictive cardiomyopathy vs. constrictive pericarditis
- Or who is being considered for cardiac transplant and needs assessment of degree and reversibility of pulmonary hypertension.
“When we first see a patient with heart failure, we try to establish hemodynamic profiles, including perfusion status, by physical examination,” says Dr. Guerrero-Miranda. “Signs include orthopnea, the presence of rales, abnormal blood pressure response to Valsalva maneuver, jugular venous pressure and abdominojugular reflex, among others. However, the sensitivity of physical exam findings is generally poor.”
A paper published in JACC: Heart Failure, July 2018, comparing the different type of clinical findings in heart failure supports the limitations of clinical findings. The highest sensitivity was found in patients with orthopnea, but specificity was higher in patients with rales. Other findings were not especially predictive.
“Overall, the positive predictive values are about 60 percent but with extremely low negative predictive values,” Dr. Guerrero-Miranda says. “All of these signs are helpful when present, but when they are absent, you cannot establish that the patient does not have acute decompensated heart failure. Hemodynamic monitoring by PAC could enable earlier detection of clinical deterioration as the guidelines suggest and expedite the escalation of therapy and/or identification of the appropriate level of mechanical support.”
The ESCAPE debate
Widespread use of the Swan-Ganz catheter, which was introduced in 1972, has been called into question by some clinicians, primarily as a result of the Evaluation study of congestive heart failure and pulmonary artery catheterization effectiveness, The ESCAPE Trial, published in JAMA in 2005
ESCAPE was a randomized controlled trial of more than 400 acutely ill patients at 26 sites who needed ICU care and hemodynamic monitoring. The inclusion criteria included patients with NYHA Class IV heart failure. However, the study excluded patients who actually may have needed a Swan: those with significant renal dysfunction (creatinine > 3.5), prior use of moderate dose inotropes, and pulmonary hypertension. In addition, the ESCAPE trial did not study patients with cardiogenic shock in whom inotropic and vasopressor therapy are frequently used or for the assessment of potential candidates for mechanical circulatory support.
“The authors of this trial dismissed the use of the Swan-Ganz when it was being used on patients with no indication, so the benefit was poor,” Dr. Guerrero-Miranda says. “When they compared the mortality benefit of using the Swan or not using the Swan, they found no difference at the end. The choice of therapies also may have influenced outcomes. Approximately 40 percent of patients in the PAC arm received inotropes.
“We have to keep in mind that PAC is a diagnostic tool. You can have the data, but if you don’t know how to interpret the data or don’t apply the therapy the data is suggesting, you may still have a poor outcome,” Dr. Guerrero-Miranda continues. “Use of the Swan helps short-term improvement of hemodynamics, but if it is not being used to transition to optimization of heart failure care, then most likely long-term outcomes are going to be poor as well. Improving heart failure outcomes requires a continuum of care.”
Hemodynamic monitoring and cardiogenic shock
In the study published in the Journal of the American Heart Association (Ranka et al in J Am Heart Assoc. 2021 Sep 7;10(17):e019843), shows that the use of PAC in cardiogenic shock is associated with improved outcomes: lower index of admission mortality, lower stroke rate, lower 30-day readmission rate, and higher left ventricular assist device implantations/orthotopic heart transplants.
Although everyone agrees that PACs should be used in cardiogenic shock, evidence supporting their optimal use has been lacking. From 2016 to 2019, eight tertiary care institutions, including Baylor University Medical Center, collected retrospective data in cardiogenic shock patients. The purpose of the study was to assess if the use of invasive hemodynamics using PAC helps to decrease mortality over time. The results of the study, published in 2020, showed that patients with complete PAC assessment had the lowest in-hospital mortality. Having no PAC assessment was associated with higher in-hospital mortality than complete PAC assessment. (Complete Hemodynamic Profiling with pulmonary artery catheters in Cardiogenic Shock is associated with lower in-hospital mortality. Garan, A.R. eta l. J Am Coll Cardiol HF, 2020; 8(11): 903-13)
#ReviveTheSwan
An analysis of a 10-year trend of PAC use and a 10-year hospitality mortality trend (2004 to 2014) shows that the use of the Swan catheter has decreased. (Hernandez GA, et al. Trends in Utilization and Outcomes of Pulmonary Artery Catheterization in Heart Failure with and without Cardiogenic Shock. J. Card Fail. 2019 May; 25(5): 354-371)
“Hopefully, this trend will begin to go up with such clear data about the efficacy of the Swan,” Dr. Guerrero-Miranda says. “In the same paper, the authors demonstrate that if we use the Swan to guide us in managing patients and then monitoring afterward, mortality is lower when the Swan was used than when it was not used.”
Publications:
Evaluation study of congestive heart failure and pulmonary artery catheterization effectiveness, The ESCAPE Trial, published in JAMA in 2005.
Ranka et al, J Am Heart Assoc. 2021 Sep 7;10(17):e019843
Complete Hemodynamic Profiling with pulmonary artery catheters in Cardiogenic Shock is associated with lower in-hospital mortality. Garan, A.R. et al. J Am Coll Cardiol HF, 2020; 8(11): 903-13