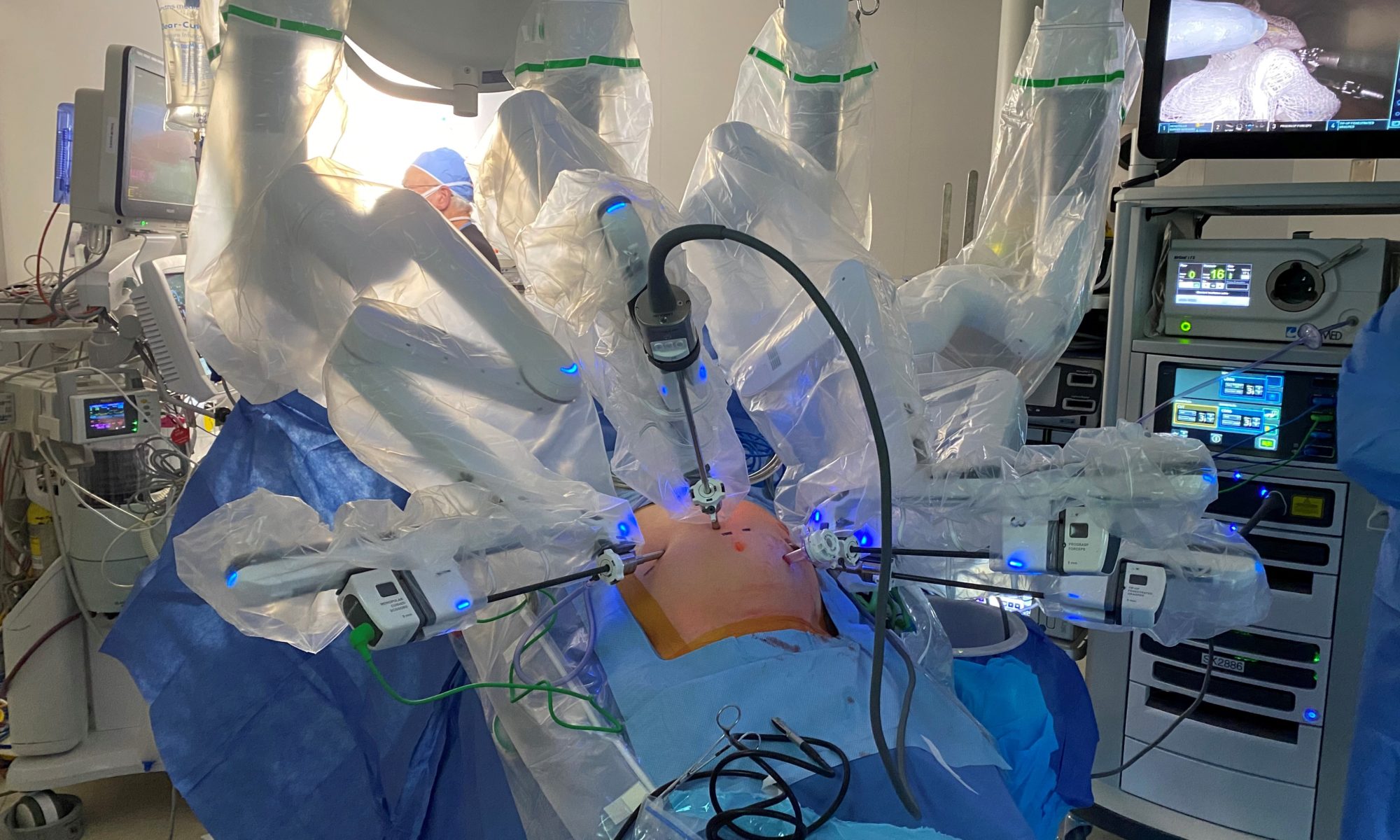
Amar Gupta, MD, FRCS(C), an abdominal transplant and hepatopancreatobiliary surgeon on the medical staff at Baylor University Medical Center, was skeptical about the benefits of the robotic surgical system in complex liver surgeries. He saw it as a gimmick, something that was more industry-driven than something that would offer a real benefit to patients. After a week’s observation of a surgeon in Riyadh, Saudi Arabia, who has performed more than 200 robotic hepatectomies, Dr. Gupta became a true believer in its value.
“I was blown away by how the robot gives a much better view and much better access to the critical structures than an open procedure,” he says. “In my opinion, these are the things that dictate the quality and safety of liver surgery. Although the robot was never designed for liver surgeries, there is a well-thought-out and calculated way to use it, making the operation very safe and very similar to open procedures.”
As with other robotic procedures, studies show there is better cosmesis and less pain than with an open procedure. Less pain translates into shorter hospital stays and a shorter time for the patient to return to work. The literature also shows there is less intraoperative blood loss with the robot than an open procedure. As with any cancer surgery, oncologic outcomes are of paramount importance, and these have been shown to be the same.
“Another major benefit with a robotic hepatectomy is the size of the incisions,” Dr. Gupta says. “In an open liver resection, the smallest incision possible is straight from the bottom of the sternum to the navel. That cut is so high it makes breathing very painful, which can be very significant in patients with lung or heart problems. The nature of liver disease means the majority of our patients are 60 or older. You generally do not want to further compromise their breathing ability.
“Using the robot, four cuts less than 1 centimeter each and one 1 centimeter cut are made for a total of five small incisions,” Dr. Gupta continues. “In some cases, a 6- to 8- centimeter cut at the bikini line, similar to a C-section, is needed in order to remove the piece of liver. This results in an easier recovery and a lower risk of hernia. The actual operative technique used for robotic hepatectomy for a malignancy or sometimes benign disease is the same technique that will be used for living liver donors.”
While robotic hepatectomy minimizes pain and recovery time for patients, the procedure is a very long and complex operation. The operative time for a robotic procedure is almost double the time required for an open procedure.
“The increased operating time and resulting soreness and fatigue for the surgeon are a small price to pay to have better recovery for patients. That’s the exact reason we want to pursue the robotic approach for living donors. Patients with cancer need the operation however it is done. Living liver donors do not. If we can minimize pain, recovery time and scarring for the donors, I think we have a responsibility to do it.”